March Is National MS Education and Awareness Month
This month, we’re focusing on Multiple Sclerosis (MS). MS involves an immune-mediated process where an abnormal response of the body’s immune system is directed against the central nervous system, which is made up of the brain, spinal cord, and optic nerves. The exact target that the immune cells are sensitized to attack remains unknown, which is why MS is considered to be “immune mediated” rather than “autoimmune.”
The cause of MS is still not known for certain, but scientists believe that the interaction of several different factors may be involved. In MS, an abnormal immune-mediated response attacks the coating around the nerve fibers in the central nervous system, as well as the nerve fibers themselves. Also, MS is known to occur more frequently in areas that are farther from the equator. Growing evidence suggests that vitamin D plays an important role, because people who live closer to the equator are typically exposed to greater amounts of sunlight year-round. Infectious factors are also being investigated; Since initial exposure to numerous viruses, bacteria and other microbes occurs during childhood, and since viruses are well-recognized as causes of demyelination and inflammation, it is possible that a virus or other infectious agent is the triggering factor in MS. While MS is not hereditary, having a first-degree relative such as a parent or sibling with MS does significantly increase an individual’s risk of developing the disease.
MS symptoms are variable and unpredictable. No two people have exactly the same symptoms, and each person’s symptoms can change or fluctuate over time. One person might experience only one or two of the possible symptoms while another person experiences many more.
More common symptoms include:
- Fatigue: Occurs in about 80 percent of people, can significantly interfere with the ability to function at home and work, and may be the most prominent symptom in a person who otherwise has minimal activity limitations.
- Walking (Gait) Difficulties: Related to several factors including weakness, spasticity, loss of balance, sensory deficit and fatigue.
- Numbness or Tingling
- Weakness
- Dizziness and Vertigo
- Sexual Problems: Very common in the general population including people with MS. Sexual responses can be affected by damage in the central nervous system, as well by symptoms such as fatigue and spasticity, and by psychological factors.
- Pain: Pain syndromes are common in MS. In one study, 55 percent of people with MS had “clinically significant pain” at some time, and almost half had chronic pain.
- Emotional Changes, including clinical depression
- Cognitive Changes: Refers to a range of high-level brain functions affected in 50 percent of people with MS, including the ability to learn and remember information, organize and problem-solve, focus attention and accurately perceive the environment.
- Bowel/Bladder Problems, including constipation or loss of bowel control
- Vision Problems: The first symptom of MS for many people. Onset of blurred vision, poor contrast or color vision, and pain on eye movement can be frightening — and should be evaluated promptly.
- Spasticity: Refers to feelings of stiffness and a wide range of involuntary muscle spasms; can occur in any limb, but it is much more common in the legs.
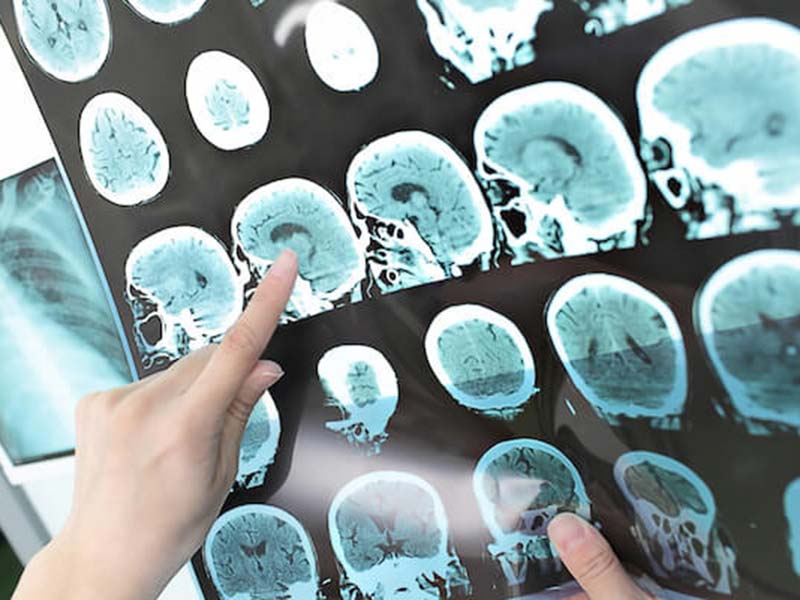
A diagnosis is made with a series of tests. Optical coherence tomography (OCT) is a relatively new, non-invasive and painless imaging tool for viewing retinal structures at the back of the eye. OCT studies have shown that the retinal nerve fiber layer is different in people with MS than in people without MS, even when there is no history of optic neuritis — making OCT a useful tool for learning more about the pathology of optic neuritis and of MS, and for gathering additional evidence of disease activity when the diagnosis of MS is suspected.
At this time, there are no symptoms, physical findings or laboratory tests that can — by themselves — determine if a person has MS. TA physician takes careful history to identify any past or present symptoms that might be caused by MS, gathers information about the birthplace, family history, environmental exposures, illness history, and places traveled, and performs a variety of tests. The doctor uses several strategies to determine if a person meets the MS diagnostic criteria. In order to make a diagnosis of MS, the physician must:
- Find evidence of damage in at least two separate areas of the central nervous system (CNS), which includes the brain, spinal cord and optic nerves AND
- Find evidence that the damage occurred at two different points in time AND
- Rule out all other possible diagnoses.
Today multiple sclerosis (MS) is not a curable disease. Effective strategies can help modify or slow the disease course, treat relapses (also called attacks or exacerbations), manage symptoms, improve function and safety, and address emotional health.
Whether it’s you or a loved one who is suffering from MS, the pain and suffering from this disease affects everyone surrounding them. Being aware of symptoms and options will help you plan treatment before a downhill struggle. If you’re seeking advice regarding MS care or are concerned that you may be expressing symptoms, contact Brevard Health Alliance.